LEPROSY
About leprosy
Leprosy is caused by the bacteria ‘Mycobacterium leprae’. It primarily affects the skin, peripheral nerves, mucosa and eyes.
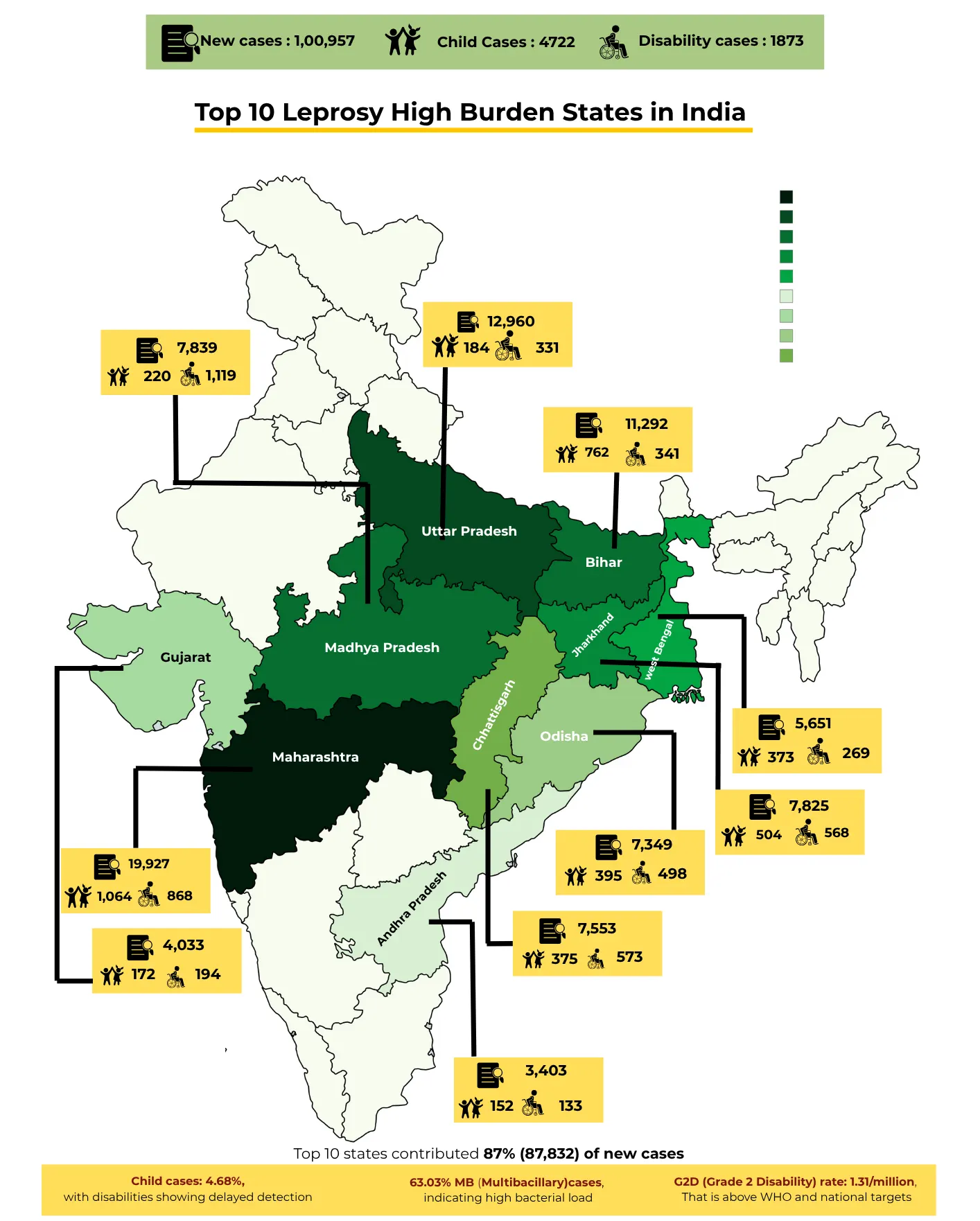
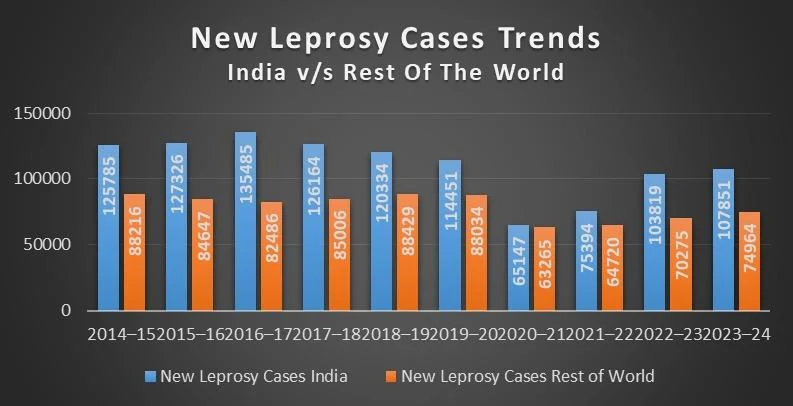
Globally, an estimated 200,000 new cases are reported each year; over half of these occurred in India.
Leprosy has been associated with significant stigma and discrimination throughout history, leading to social isolation and exclusion.
Leprosy continues to be one of the major causes of permanent disability in India. A large number of people with disabilities due to leprosy need a continuum of care.
India hosts over half of the global leprosy-affected population living in tribal, rural and neglected geographies.
One consequence in India, is that India has over 700 isolated leprosy colonies. In these colonies people largely live in vulnerable conditions, unhealthy environments, and facing ongoing discrimination and stigma.
Overall Leprosy is still an isolating disease, causing immense distress to individuals and families of affected people… impacting lives – physically, mentally, socially and economically; and worse: leprosy is still feared by most people in society.
History:
- Leprosy has affected humanity for thousands of years, with historical records dating back to ancient civilizations.
- In the Middle Ages (1,300-1,500) leprosy was often associated with divine punishment and moral decay, leading to segregation and isolation of affected individuals.
- The discovery of effective treatment with antibiotics in the mid-20th century revolutionised by offering cure, shifting focus from isolation to rehabilitation and social integration.
Symptoms:
- Skin lesions: Hypopigmented or erythematous patches with decreased sensation.
- Signs of infectious leprosy include thickened skin / nerves, oily face, eyebrow loss, & earlobe / face nodules.
- Nerve damage: Sensory loss, muscle weakness, and paralysis due to peripheral nerve involvement.
- Eye involvement: leprosy affects facial nerve / eyes; untreated leads to vision impairment & blindness.
Transmission:
- Transmission primarily occurs through airborne droplet infection from untreated individuals.
- Incubation period ranges from months to years, making it challenging to trace the source of infection.
- Risk of transmission is from untreated infectious leprosy patients.
- There is no protective vaccine to stop the transmission and spread of leprosy in the community.
Epidemiology:
- Despite significant progress in reducing the global burden, leprosy persists as a public health concern in many regions.
- Leprosy prevalence is high in several countries, with the highest burden in India, Brazil, and Indonesia.
- The Covid-19 pandemic further exacerbated the problem as annual case registration dropped by 48% in 2020-21, 40% in 2021-22 and 18% in 2022-23. This has led to continued disease transmission, and more child and disability cases due to non or delayed detection.
Diagnosis:
- Early diagnosis is crucial to prevent the spread, nerve damage and disabilities.
- Diagnosis is primarily clinical, based on examination of skin and nerves.
- Lab tests, such as slit skin smears or biopsies, confirm the presence of leprosy bacteria and help determine infectivity and outcome.
Treatment:
- Multidrug Therapy (MDT) is the cornerstone of leprosy treatment, consisting of a combination of antibiotics such as dapsone, rifampicin, and clofazimine.
- MDT, highly effective with cure rates exceeding 95%. It is provided free by WHO to endemic countries, resulting in cure, prevalence reduction, and transmission decline.
- MDT treatment is provided free in India at primary health centres (PHCs) and public hospitals.
Prevention:
- Prevention strategies focus on early detection, prompt treatment, and contact tracing to interrupt chain of transmission including disability management and care.
- Health education, public engagement, and dissemination of scientific facts remove irrational fear and prejudice.
- Community involvement reduces stigma, promotes inclusion for affected individuals and families.
Stigma and discrimination:
- Despite medical advances and effective treatment, misconceptions about the disease persist, contributing to social marginalisation.
- Stigma reduction requires community engagement, education, and advocacy to promote acceptance, inclusion and mainstreaming.
Advocacy:
- Advocacy efforts are needed to raise awareness, promote self-reporting and reduce stigma; ensuring access to quality care for all individuals affected by leprosy.
Research:
Organisations such as WHO, Leprosy Research Initiative and research institutions worldwide are committed to leprosy research, advocacy, and support.
Research priorities include developing new drugs, improving diagnostic tools, understanding how the disease develops, and addressing social determinants of health.
*
Reference links: